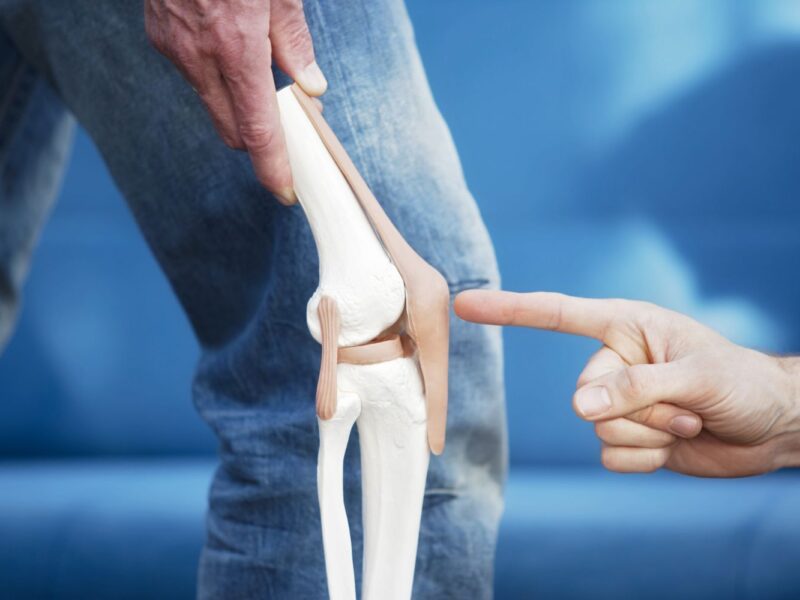
The knee cap, or patella, is a small bone situated at the front of the knee joint. Despite its modest size, the patella plays a crucial role in knee function, facilitating movement, stability, and load distribution.
However, various factors can lead to conditions and injuries affecting the patella, causing pain, instability, and functional impairment. In this comprehensive guide, we explore the most common patellar conditions and injuries, including their causes, symptoms, diagnosis, and treatment options.
Patellar Dislocation/Subluxation
Patellar dislocation occurs when the patella moves out of its normal alignment within the patellofemoral groove, either partially (subluxation) or completely. This displacement can result from sudden twisting motions, direct blows to the knee, or underlying anatomical abnormalities.
Symptoms: Acute pain, swelling, visible deformity, and difficulty straightening the knee characterize patellar dislocation. Patients may report a sensation of the knee giving way or locking.
Diagnosis: Physical examination, including evaluation of patellar tracking and stability, along with imaging studies such as X-rays or MRI, confirms the diagnosis.
Treatment: Initially, the focus is on reducing pain and swelling through rest, ice, compression, and elevation (RICE). Physical therapy to strengthen surrounding muscles and improve joint stability is crucial for long-term management. Severe or recurrent dislocations may require surgical intervention to realign the patella and repair damaged structures.
Patellar Fracture
Patellar fractures range from small cracks to complete breaks and typically result from direct trauma or high-impact injuries such as falls or sports-related collisions. Fractures may involve the patellar body or its bony attachments to the quadriceps or patellar tendons.
Symptoms: Pain, swelling, bruising, and difficulty bearing weight on the affected leg are common signs of a patellar fracture. Severe fractures may cause visible deformity or inability to extend the knee.
Diagnosis: X-rays are the primary diagnostic tool for identifying patellar fractures. Additional imaging, such as CT scans, may be necessary to assess complex fractures or associated soft tissue injuries.
Treatment: Treatment depends on the severity and stability of the fracture. Non-displaced or minimally displaced fractures may heal with conservative measures like immobilization, followed by physical therapy. However, displaced fractures or those involving tendon avulsion may require surgical fixation to restore alignment and function.
Patellar Tendonitis (Jumper’s Knee)
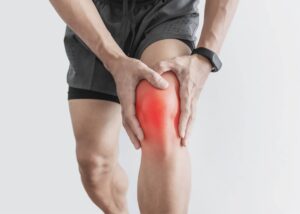
Patellar tendonitis, also known as jumper’s knee, is an overuse injury characterized by inflammation and degeneration of the patellar tendon, which connects the patella to the tibia. Repetitive stress from activities like jumping, running, or squatting can lead to microtrauma and tendon damage.
Symptoms: Pain, tenderness, and swelling around the lower pole of the patella are hallmark symptoms of patellar tendonitis. Pain typically worsens with activity and may improve with rest. Diagnosis: Diagnosis is based on clinical evaluation, including a thorough history of symptoms and physical examination. Imaging studies like ultrasound or MRI may be ordered to assess tendon integrity and rule out other pathology.
Treatment: Initial treatment involves rest, activity modification, and anti-inflammatory measures to reduce pain and inflammation. Physical therapy focusing on eccentric strengthening exercises, flexibility training, and biomechanical corrections is essential for tendon rehabilitation. In refractory cases, corticosteroid injections or extracorporeal shockwave therapy may be considered. Surgery is rarely indicated and reserved for severe cases of tendon degeneration or rupture.
Chondromalacia Patellae
Chondromalacia patellae refers to the softening and degeneration of the cartilage beneath the patella, leading to pain, crepitus, and functional limitations. It often results from abnormal patellar tracking, malalignment, or biomechanical factors causing increased pressure on the patellofemoral joint.
Symptoms: Anterior knee pain, particularly with activities like climbing stairs, kneeling, or prolonged sitting, is a common complaint in individuals with chondromalacia patellae. Swelling and grinding sensations (crepitus) may also be present.
Diagnosis: Diagnosis is based on clinical symptoms, physical examination findings, and imaging studies such as X-rays, MRI, or arthroscopy to assess cartilage damage and joint integrity. Treatment: Conservative management is the mainstay of treatment for chondromalacia patellae and includes rest, activity modification, quadriceps strengthening exercises, and patellar taping to improve tracking. Physical therapy modalities such as ultrasound, electrical stimulation, and joint mobilization may provide symptomatic relief. In severe cases, refractory to conservative measures, arthroscopic surgery may be indicated to address cartilage damage, correct alignment issues, or release tight soft tissues.
Conclusion
Common knee cap (patella) conditions and injuries encompass a spectrum of pathologies ranging from acute traumatic dislocations to chronic overuse syndromes like patellar tendonitis and chondromalacia patellae.
Early recognition, accurate diagnosis, and prompt intervention are essential for optimizing outcomes and preventing long-term complications. By implementing a tailored treatment approach that combines conservative measures, rehabilitative interventions, and surgical options when necessary, healthcare providers can effectively manage patellar-related issues and restore function and quality of life for affected individuals.
Related Tags
Taiwo Olawuyi
Taiwo Olawuyi is a highly dedicated and passionate professional blogger, renowned for her ability to create captivating, informative, and engaging content in the realm of health and wellness. She holds a Bachelor's degree in Political Science from Olabisi Onabanjo University and a Master's degree in Adult Education from the prestigious University of Ibadan. Her profound passion for health and wellness, coupled with her unwavering dedication to her audience, serves as a constant source of inspiration and enlightenment for readers worldwide.