Pregnancy presents a unique challenge in the diagnosis and management of appendicitis. Appendicitis is one of the most common non-obstetric surgical emergencies encountered during pregnancy, with potentially serious consequences for both the mother and the fetus.
However, the diagnosis of appendicitis in pregnant women is often complicated by overlapping symptoms with normal pregnancy changes and concerns about radiation exposure from imaging studies. In this essay, we will explore the challenges in diagnosing and treating appendicitis during pregnancy, as well as strategies for optimizing outcomes for both the mother and the fetus.
Understanding Appendicitis in Pregnancy
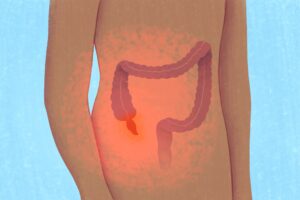
Appendicitis is caused by inflammation of the appendix, a small pouch attached to the colon, typically due to obstruction of the appendiceal lumen by fecaliths, lymphoid hyperplasia, or tumours. The classic symptoms of appendicitis include right lower quadrant abdominal pain, nausea, vomiting, and fever. However, these symptoms can be nonspecific and overlap with common complaints of pregnancy, such as round ligament pain, gastrointestinal upset, and uterine contractions.
Challenges in Diagnosis
Diagnosing appendicitis during pregnancy can be challenging due to the physiological changes that occur in the abdomen and pelvis during gestation. The enlarging uterus displaces the appendix superiorly and laterally, leading to atypical presentation of symptoms and difficulty in localizing tenderness on physical examination.
Moreover, concerns about fetal radiation exposure limit the use of imaging modalities traditionally used for diagnosing appendicitis, such as computed tomography (CT) scans. Clinical assessment and laboratory investigations play a crucial role in the initial evaluation of suspected appendicitis in pregnant women.
However, relying solely on clinical judgment can delay diagnosis and increase the risk of complications. Therefore, a high index of suspicion is warranted, and prompt diagnostic evaluation is essential to prevent delays in treatment.
Imaging Modalities and Radiation Concerns
Imaging studies are an integral part of the diagnostic workup for appendicitis in non-pregnant patients, with CT scans being the gold standard due to their high sensitivity and specificity. However, the use of CT scans in pregnant women is limited due to concerns about radiation exposure to the fetus, particularly during the first trimester when organogenesis occurs.
Ultrasound is the preferred imaging modality for evaluating suspected appendicitis in pregnant women due to its safety and availability. However, ultrasound has lower sensitivity and specificity compared to CT scans, particularly in obese patients and those with anatomic variations.
Magnetic resonance imaging (MRI) is another option for pregnant women, offering excellent soft tissue contrast without radiation exposure. However, MRI may not be readily available in all clinical settings and may be contraindicated in patients with certain implants or devices.
Management Considerations
Once the diagnosis of appendicitis is confirmed or strongly suspected in a pregnant woman, prompt surgical intervention is generally recommended to minimize the risk of complications, such as perforation and peritonitis.
Delaying surgery increases the risk of fetal and maternal morbidity and mortality. Laparoscopic appendectomy is the preferred surgical approach, as it is associated with shorter hospital stays, fewer complications, and faster recovery compared to open surgery.
However, the decision to proceed with surgery must balance the risks and benefits to both the mother and the fetus. The timing of surgery, the choice of surgical approach, and intraoperative fetal monitoring should be carefully considered in consultation with a multidisciplinary team, including obstetricians, general surgeons, and anesthesiologists.
In cases where surgery is contraindicated or deferred, conservative management with antibiotics may be considered under close observation. However, this approach carries a higher risk of perforation and abscess formation and should be reserved for cases where surgical intervention is not feasible or safe.
Conclusion:
Appendicitis during pregnancy presents unique challenges in diagnosis and management, requiring careful consideration of maternal and fetal well-being. Healthcare providers must maintain a high index of suspicion for appendicitis in pregnant women presenting with abdominal pain and other nonspecific symptoms.
Prompt diagnostic evaluation, including clinical assessment, laboratory investigations, and appropriate imaging studies, is essential to facilitate timely intervention and prevent complications.
The choice of imaging modality should prioritize safety and minimize radiation exposure to the fetus, with ultrasound and MRI being preferred over CT scans whenever possible. Surgical intervention, preferably laparoscopic appendectomy, is generally recommended for confirmed or strongly suspected cases of appendicitis to minimize maternal and fetal risks.
However, the decision to proceed with surgery must be individualized based on the clinical presentation, gestational age, and maternal-fetal status, with close consultation with a multidisciplinary team.
By recognizing the challenges associated with diagnosing and managing appendicitis during pregnancy and implementing appropriate strategies, healthcare providers can optimize outcomes for both the mother and the fetus, reducing the risk of complications and ensuring the best possible care for pregnant women with appendicitis.