Jaundice is a common condition in newborns characterized by the yellowing of the skin and eyes due to elevated levels of bilirubin in the blood. While mild jaundice is common and often resolves on its own, severe jaundice can lead to serious complications such as brain damage.
Therefore, monitoring and managing bilirubin levels in newborns are crucial aspects of neonatal care. This essay explores the various methods of monitoring and managing bilirubin levels in newborns, including assessment tools, treatment options, and preventive measures.
Assessment of Bilirubin Levels
Monitoring bilirubin levels in newborns involves both clinical assessment and laboratory testing. Clinical assessment includes visual inspection of the skin and mucous membranes for signs of jaundice. The extent of jaundice is typically graded based on the area of the body affected and the intensity of the yellowing.
In addition to clinical assessment, laboratory testing is essential for accurate measurement of bilirubin levels. The most common method is serum bilirubin testing, which involves obtaining a blood sample from the newborn and analyzing it for total serum bilirubin (TSB) concentration. TSB levels can be measured using various techniques, including spectrophotometry and direct or indirect bilirubin assays.
Another important tool for assessing bilirubin levels in newborns is transcutaneous bilirubinometry (TCB). This non-invasive method uses a handheld device to measure bilirubin levels through the skin, providing a quick and convenient way to screen for jaundice. Although TCB measurements may not be as accurate as serum bilirubin testing, they can help identify infants at risk of severe jaundice who require further evaluation.
Management of Neonatal Jaundice
The management of neonatal jaundice depends on various factors, including the severity of jaundice, the underlying cause, and the presence of risk factors for bilirubin-induced neurotoxicity. Mild jaundice in otherwise healthy-term infants may not require any treatment and can often be managed with close monitoring and supportive care.
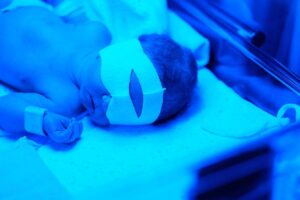
For infants with moderate to severe jaundice or those at risk of complications, treatment options include phototherapy and exchange transfusion. Phototherapy involves exposing the newborn’s skin to blue or white light, which helps convert bilirubin into a water-soluble form that can be excreted from the body. Phototherapy can be delivered using overhead lights or specialized devices such as blankets or beds with built-in light sources.
In cases where phototherapy is ineffective or contraindicated, exchange transfusion may be necessary. This procedure involves removing a portion of the newborn’s blood and replacing it with donor blood or plasma to reduce the concentration of bilirubin. Exchange transfusion is typically reserved for infants with severe jaundice or those who do not respond to other treatments.
Preventive Measures
Preventing severe jaundice in newborns requires early identification of infants at risk and appropriate interventions to minimize bilirubin levels. Antenatal risk factors for neonatal jaundice include maternal diabetes, blood group incompatibility, and certain medications taken during pregnancy. Identifying these risk factors during prenatal care allows healthcare providers to monitor newborns closely after birth and intervene promptly if jaundice develops.
Another important preventive measure is promoting breastfeeding, as breast milk jaundice is a common cause of prolonged jaundice in breastfed infants. While breastfeeding should be encouraged for its numerous benefits, healthcare providers should educate parents about the signs of breastfeeding-associated jaundice and provide support to ensure adequate milk intake and weight gain.
Conclusion
Monitoring and managing bilirubin levels in newborns are essential aspects of neonatal care aimed at preventing complications associated with severe jaundice. Clinical assessment, laboratory testing, and non-invasive screening tools such as transcutaneous bilirubinometry are used to evaluate bilirubin levels and identify infants at risk.
Treatment options for neonatal jaundice include phototherapy and exchange transfusion, with preventive measures focusing on early identification of risk factors and promoting breastfeeding. By implementing comprehensive strategies for monitoring and management, healthcare providers can ensure optimal outcomes for newborns affected by jaundice.
Related Tags
Taiwo Olawuyi
Taiwo Olawuyi is a highly dedicated and passionate professional blogger, renowned for her ability to create captivating, informative, and engaging content in the realm of health and wellness. She holds a Bachelor's degree in Political Science from Olabisi Onabanjo University and a Master's degree in Adult Education from the prestigious University of Ibadan. Her profound passion for health and wellness, coupled with her unwavering dedication to her audience, serves as a constant source of inspiration and enlightenment for readers worldwide.