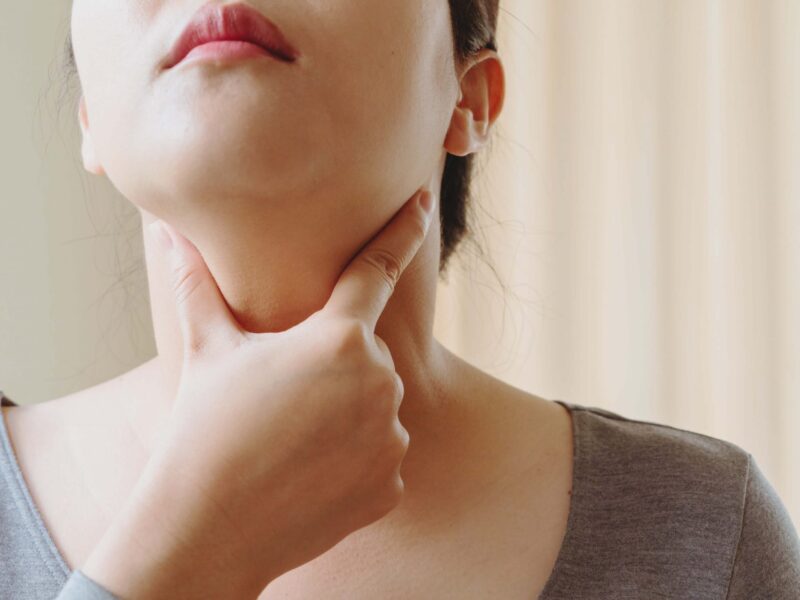
Goitre, also spelt as goitre, is a medical condition characterised by the abnormal enlargement of the thyroid gland, which is a butterfly-shaped gland located in the front of the neck, just below Adam’s apple (in men) or the laryngeal prominence (in women). This condition can be caused by various factors and may result in a range of symptoms.
Causes
- Iodine Deficiency: Historically, iodine deficiency was a leading cause of goitre worldwide. Iodine is essential for the production of thyroid hormones, and a lack of it can lead to thyroid enlargement. However, iodine deficiency goitre is now rare in areas with iodized salt programs.
- Autoimmune Thyroid Disorders: Conditions like Hashimoto’s thyroiditis, an autoimmune disorder, can cause chronic inflammation of the thyroid gland, leading to goitre.
- Graves’ Disease: Another autoimmune disorder, Graves’ disease, can stimulate the thyroid to produce excessive amounts of hormones, leading to gland enlargement.
- Nodular Goitre: This type of goitre occurs when one or more nodules or lumps develop within the thyroid gland. These nodules can be non-cancerous (benign) or cancerous (malignant).
- Subacute Thyroiditis: Infections or inflammation of the thyroid gland can result in goitre, which is usually painful and may resolve on its own.
- Certain Medications: Some medications, particularly those that contain iodine or interfere with thyroid function, may contribute to goitre development.
Symptoms

The severity and nature of symptoms can vary depending on the cause and size of the goitre. Common symptoms include:
- Visible swelling in the neck.
- Difficulty swallowing or breathing, especially if the goitre is large.
- Hoarseness of the voice.
- Neck discomfort or pain, especially when turning the head or wearing tight collars.
In some cases, goitre may not cause noticeable symptoms, or symptoms may be subtle and develop gradually.
Diagnosis
The diagnosis of goitre typically involves:
- Physical Examination: A healthcare provider will examine the neck to assess the size and characteristics of the goitre.
- Blood Tests: Thyroid function tests, such as TSH (thyroid-stimulating hormone), T3, and T4 levels, are assessed to evaluate thyroid function.
- Imaging: Ultrasound, CT scans, or MRI may be used to visualize the thyroid gland, determine the size of the goitre, and identify any nodules.
- Fine-Needle Aspiration (FNA): If nodules are present, an FNA biopsy may be performed to determine if they are cancerous or benign.
Treatment
The treatment of goitre depends on its cause, size, and associated symptoms:
- Iodine Supplementation: In cases of iodine deficiency, providing iodine supplements or ensuring an iodine-rich diet may resolve the goitre.
- Medication: In cases of inflammation or autoimmune disorders, medications like corticosteroids or thyroid hormone replacement therapy may be prescribed.
- Surgery: If the goitre is causing severe symptoms, proliferating, or if nodules are suspected to be cancerous, surgical removal of part or all of the thyroid gland may be necessary.
- Radioactive Iodine Therapy: This treatment is used to shrink the thyroid gland, particularly in cases of hyperthyroidism associated with goitre.
- Observation: Small, asymptomatic goitres may be monitored with regular check-ups.
Prevention
- Ensure a diet with sufficient iodine, either through iodized salt or iodine-rich foods (e.g., seafood, dairy, and fortified products).
- If you have an autoimmune thyroid disorder, work closely with your healthcare provider to manage the condition effectively.
- Please check your neck for any unusual changes or swelling.
Goitre is a treatable condition, and early diagnosis and intervention are essential to prevent complications and ensure proper management.
If you suspect you have a goitre or experience symptoms related to thyroid issues, consult a healthcare professional for a thorough evaluation and personalized guidance.